Breastfeeding and depression: It’s complicated
A recent Facebook post by Jack Newman has elicited passionate discussion about the relationship between breastfeeding and postpartum depression. Dr. Newman posted an email he’d received yesterday:
My baby is 3 months old and breastfeeding has been “bliss” for me so far. We both enjoy our relationship and it is very important for me as I have postpartum depression and right now breastfeeding is the only thing that works as I would have hoped and planned. (My comment: Many mothers tell me that they are told to stop breastfeeding for medication for postpartum depression and say that they are so upset because “breastfeeding is the only thing in their life that is working”. Do doctors ever think of this?).
I’m happy to report that I’m a doctor, and I do think of this — in fact, at UNC, we’re starting a 5-year NIH-funded study to try to understand the relationship between breastfeeding, postpartum depression, and infant attachment. Our pilot data suggest that this relationship is complicated. We recruited 52 women who were intending to breastfeed and either did or did not have a history depression and/or anxiety. During pregnancy, mothers provided baseline blood samples, completed questionnaires, and had a standardized psychiatric interview to assess their history. Mothers came to our lab with their babies at 2 and 8 weeks postpartum, and we measured hormone levels while they breastfed their babies.
During pregnancy, we found that mothers who had higher levels of the hormone oxytocin had lower scores on the EPDS, a standard measure of depression, consistent with another recent study of oxytocin and mood symptoms. When mothers returned at 2 weeks, we did not find any relationship between mood and hormone levels during breastfeeding, but at 8 weeks, the mothers with higher depression and/or anxiety had lower levels of oxytocin during breastfeeding (see figure). They were also less happy, and more stressed, depressed, irritated and overwhelmed, during the entire feeding visit than mothers who were not anxious or depressed.
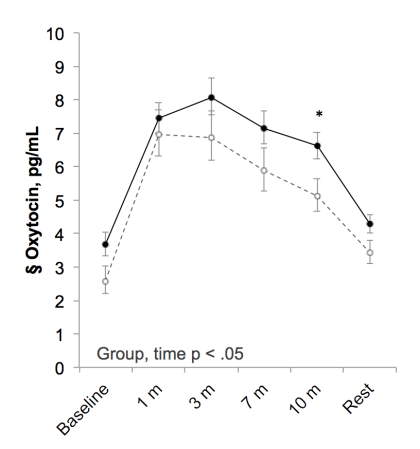
Maternal neuroendocrine response to feeding 8 weeks among women with depression/anxiety symptoms (dashed line) or without mood symptoms (solid line).
These results raise some interesting questions about the conventional wisdom that breastfeeding prevents depression. It could be that mothers who have lower oxytocin levels have trouble with breastfeeding and also feel more anxious and depressed. Or it could be that, for mothers whose baseline oxytocin is lower, breastfeeding gives them a boost that’s essential for them to feel connected to their babies.
There is also provocative evidence that oxytocin may increase stress in some individuals. A study of men who were or were not separated from a parent in childhood found that a dose of inhaled oxytocin actually increased levels of the stress hormone cortisol among the men who had experienced early parental separation. In a small study in Australia, depressed mothers were treated with inhaled oxytocin at one lab visit and placebo at another visit. When mothers received oxytocin, they were more likely to describe their infants as difficult, and were sadder, but also reported a more positive relationship with their infant. The study included mothers of infants who were 3-12 months old, and 40% of the women in the study were breastfeeding at the time of the visit. It’s not clear whether the effect of oxytocin would be different in a group of mothers who were all breastfeeding. However, these results suggest that the oxytocin increase triggered by breastfeeding may worsen anxiety and depression for some mothers. In our five-year study, we will explore these issues in a larger sample — we plan to recruit 234 women and follow them and their infants through 12 months postpartum.
The nuances of the biology suggest that doctors absolutely need to think about the effect of breastfeeding on a woman’s mood symptoms — and that the effect likely differs from mother to mother. I have cared for women with postpartum depression who describe breastfeeding as the only thing that ties them to their baby. I’ve also cared for women who are struggling with milk production and spending all of their time trying to eek out a few more drops of breast milk, at the expense of their baby’s other needs. One mother, who came to see me during her second pregnancy to talk about strategies to optimize breastfeeding, recalled one day when her first baby was 4 months old. He was lying on the floor, screaming, and she was ignoring his cries because she was busy pumping. She said she realized, at that moment, that she needed to prioritize mothering over making milk.
We have much more work to do to understand the biology of postpartum depression. However, when a mother is experiencing depression and anxiety symptoms, my job as a clinician is to ask her what parts of her day bring her joy and peace, and what makes her symptoms worse. I need to ask her how breastfeeding is going — and listen, without judgment, to her answer. If breastfeeding is the lifeline that is holding her and her baby together, then we’ll build her treatment around protecting that breastfeeding relationship. Conversely, if she grits her teeth for every feeding and counts the minutes until it is over, then breastfeeding may be contributing to her symptoms and hurting her relationship with her baby. We need to talk about why breastfeeding is stressful, and whether there are strategies that can make the experience better — or whether she and her baby would be better served if she weaned. On a population level, not breastfeeding is associated with risks of both maternal and infant disease. On an individual level, however, a doubling in the risk of an ear infection may be a reasonable tradeoff for a doubling of mom’s dislike of her baby, eight to ten times every day.
So in answer to Dr. Newman’s post — yes, doctors do “ever think about this.” More importantly, we need to take the time to talk about it with each mother that we see. We need to explore what breastfeeding means for her, and we need to tailor our recommendations to her needs in order to reduce her depression symptoms and strengthen her relationship with her baby.
Alison Stuebe, MD, MSc, is a maternal-fetal medicine physician, breastfeeding researcher, and assistant professor of Obstetrics and Gynecology at the University of North Carolina School of Medicine. She is a member of the board of the Academy of Breastfeeding Medicine.
Posts on this blog reflect the opinions of individual ABM members, not the organization as a whole.



The mothers who have depression/anxiety – were they taking medication or unmedicated? If not taking mediations, were they on them before, during or after their pregnancies?
Amber
May 30, 2013 at 11:44 am
Some mothers were taking medication and some were not. We looked at oxytocin during feeding at 8 weeks as a function of both symptoms and medication use, and we found the lowest oxytocin levels among the mothers who were taking medication but still had symptoms. This may be because the group that was resistant to treatment included the women with the most severe underlying disease.
astuebe
May 30, 2013 at 11:49 am
interesting study! I have breastfed all three of my babies and have noticed an increase in anxiety when my milk production decreases and when my babies wean. I find that nursing helps me to take a timeout during the day to relax and focus on me and baby.
Traci Eggleston
May 30, 2013 at 6:22 pm
I’m so glad you’re looking at this! The interplay between postpartum mood disorders and breastfeeding is something I’m really interested in.
One thing I’d like to see explored – or maybe it has been and you can link me to studies – is the relationship of perceived insufficient milk supply and depression/anxiety (whether diagnosed or not). Just from observing moms, it seems that breastfeeding and milk supply can be used as scapegoats of sorts, with a mom focusing on her milk supply (which seems sufficient because baby is growing well) in a way that doesn’t make sense and seems like it could be an outlet for anxiety.
Tiffany Gallagher
May 31, 2013 at 9:15 am
I breastfeed. I actually went off my anti depressant at 6-8 weeks because they made my post partum worse. Now at 6 1/2 months, I am going to be going back on them, because dealing with the post partum has become more difficult. It is such a tenuous thing to deal with.
findingtheearth
May 31, 2013 at 9:22 am
Breastfeeding my 2nd was miserable at first, until I figured out I was experiencing “dysmorphic milk ejection reflex.” Knowing it was okay to ride out the “depression attack” and that it was something chemical happening in me helped me so much, and I’m pretty sure I didn’t experience actual ppd as a result.
Jenn
May 31, 2013 at 10:58 am
I am sorry Alison, but I think that the paragraph that starts with “The nuances of biology…” is exactly what is wrong with how we think about breastfeeding. We have done a very good job of “selling” breastmilk, but a very poor job of “selling” breastfeeding. In other words, by breastfeeding I mean feeding the baby at the breast, not providing breastmilk elsewhere than at the breast. Thus, in many instances, mothers are enjoined to pump as much as possible to increase the milk available to the baby. The mothers are made to feel that if they cannot pump enough, then they are just not doing their job as mothers. This is a boon for the pump manufacturers but not for the mothers or babies. As one mother told us when attending our clinic, “Pumping takes away your will to live”. It was a joke, but behind every joke is a truth.
About the “one mother who came” to see you, Alison, in our clinic we would have approached the problems in a different way. If the mother is already supplementing with formula, we suggest that she not pump. For the following reasons:
1. Pumping is expensive (to rent or buy the machine).
2. Pumping is tiring and time consuming.
3. Pumping diminishes the mother’s enjoyment of breastfeeding.
4. Pumping, if not done properly, may cause sore nipples.
5. In spite of everything we tell mothers, that you cannot tell how much you are producing or can produce, mothers look at what they pump and get discouraged.
6. Pumping puts the emphasis on breastmilk as a product. And pumping causes mothers to concentrate on delivering the product rather than on breastfeeding, which is why the four month old in your blog is on the floor crying instead of at the breast content.
7. Breastfeeding is much more than breastmilk.
We would have encouraged the “ideal” latch. We would have taught the mother how to know the baby is actually getting milk (see the video clips at our website http://www.breastfeedinginc.ca). We would have taught the mother to use breast compression to increase the flow of milk to the baby, which is, in a way, like pumping except that the milk goes to the baby instead of to a bottle. In addition, we would have shown the mother how to use a lactation aid at the breast so that the baby is supplemented while breastfeeding, not after a feeding (or in some cases before the feeding, as some suggest, to my astonishment).
In conclusion, I will reiterate that the goal is breastfeeding, not breastmilk. When we emphasize breastmilk, we have completely misunderstood the biology of infant feeding.
Jack Newman
June 1, 2013 at 7:15 am
I really think that if you have starting to compliment with formula you need to express using a breastpump to increase your supply. (Is there any research done on whether use of lactation aid alone will increase the supply enough) It is worth the effort in many cases especially if using motilium.
I have breastfed two children but lost my supply with my first at 3 months. I would have loved to have been given the opportunity to use a breastpump. 30 years ago I was not given the advise or opportunity which the Mums have today (I only had a rubber ball ended devise which was useless.) I think your research on postnatal looks great and makes a lot of sense. I must say that although I am a very anxious person breastfeeding my children was one of the happiest and fullfilling times in my life and I now try to help Mums to continue as long as they possibly can. I fed my 2nd child until she was over 3 yrs old. We are forever learning in this field. Julie LC
Julie
June 17, 2013 at 10:48 pm
Jack Newman
I am so excited to see your post. You have hit the nail on the head as far as I’m concerned. I am impressed!
I am no maternal-child expert, I am a nurse anesthetist by trade. I have, however, nursed my four infants successfully. Hard to trust yoyr infant is Okay, if they are fussing and people are tellibgbyou tgeyre hungry. i would let my husband (a pediatrician) offer a bottle of formula after i nursed. when the baby rejected the additional feed we were both assured it was not lack of nutrition, but rather just beibg a baby!:). I pumped at work, begrudgingly:), two days a week. It did what I needed, but agree with you whole heartedly. Pumping is not nursing. I do experience mood swings at the cessation of breast feeding which I actually dread. They have typically lasted two weeks. I do not treat with anything other than exercise and hugs!
Holly
Holly leischner
January 11, 2014 at 8:54 am
Sorry for typos on cell phone
Holly leischner
January 11, 2014 at 8:56 am
[…] Allaitement et dépression. […]
A tire d'Ailes | Revue de presse allaitement
June 27, 2013 at 3:05 am
Dr Jack, you comments on not pumping if mum is already using formula make great sense and is so much hard work. I wish the use of supplementers was more widely recognised. Love your work!
Shirley
June 28, 2013 at 5:47 am
[…] at the University of North Carolina School of Medicine Alison Stuebe, MD, MSc recently wrote Breastfeeding and depression: It’s Complicated, a fascinating post on the Academy of Breastfeeding Medicine’s blog. Her work is of such value […]
OB/GYN sheds light on creating breastfeeding culture | Our Milky Way
July 7, 2013 at 4:31 pm
For me, the first 2 weeks were good because I did not know my supply was low, or that my baby was dehydrated and underweight. Everything fell apart when I found out and tried to get my supply up. Nursing became stressful because I had to take my baby outside naked in January to keep her awake at an empty breast. Pumping 10x a day meant I could no longer sleep while the baby slept, and I cancelled my daily walks because i couldn’t leave the house — so I was way more sleep deprived and isolated. I gave her formula via SNS system, which messed up the baby’s latch, and my nipples were bleeding. I started taking Reglan, which has a possible side-effect of depression. I disengaged from my baby while pumping, ignoring her crying because “I can’t say I really tried if I stop pumping.” Instead I just watched the little drops slowly plunk into the pump bottles and daydreamed about cutting my wrists and making my blood flow like the milk wouldn’t. I had those fantasies 10 times a day.
Looking back, I’d be shocked if I hadn’t become depressed. 8 months later I’m still on antidepressants.
Erin
August 22, 2013 at 1:11 am
[…] Breastfeeding and depression: It's complicated | Breastfeeding … […]
Prenatal depression linked to child's depression later in life | Depression: What about it?
October 23, 2013 at 8:13 pm
Do you know of any study that address whether weaning per se (w/associated endocrine or hormonal changes) does or does not bring on depression in some women? Is there is any research on whether it is better to wean gradually or abruptly in order to minimize susceptibility to weaning depression? (I am especially interested in a particular case of weaning a 5-6 month old baby.)
jean
October 27, 2013 at 10:05 am
[…] We’ll be chatting with none other than the fabulous Dr. Samantha Meltzer-Brody and Dr. Alison Stuebe, both with UNC’s Perinatal Psychiatry Unit. This is a ground-breaking program here in the United States for women struggling with Perinatal Mood Disorders. They are currently focusing on research which examines the biology behind the relationship behind depression and breastfeeding. Dr. Stuebe writes: […]
Announcing the #PPDChat Guests for 11.13.13: Drs. Samantha Meltzer-Brody & Alison Stuebe | My Postpartum Voice
November 8, 2013 at 10:55 am
[…] Breastfeeding and depression: It's complicated | Breastfeeding … […]
Training May Help Autism Moms Reduce Stress – Disability Scoop | Alternative Depression Treatments
November 12, 2013 at 1:11 am
[…] Breastfeeding and depression: It's complicated | Breastfeeding … […]
Out of the darkness: A story of Hope, love and courage – The Border Mail | Alternative Depression Treatments
November 22, 2013 at 8:22 am
[…] Breastfeeding and depression: It's complicated | Breastfeeding … […]
Holiday depression: How to cope with the holiday blues – The Grio | Alternative Depression Treatments
December 6, 2013 at 8:34 pm
[…] Breastfeeding and depression: It's complicated | Breastfeeding … […]
Female libido drug remains in limbo | Depression: What about it?
December 15, 2013 at 8:22 pm
Thank you for your research! In my personal experience breastfeeding (even when it goes well) can contribute to depression. I am currently (successfully) breastfeeding my third child but I have postpartum depression. I also breastfeed my two older children and experienced postpartum depression after each of their births. The depression went away shortly after weaning each time. I wish more was done to investigate the links between body chemistry, breastfeeding, and depression in the postpartum period.
Heather
December 16, 2013 at 4:09 pm
Thank you for your article. I suffer from pod and just had my second child. Breastfeeding my children has always stressed me out. I felt as though they were never satisfied and that they were latched on constantly. Every time I breastfed it felt as if I lost part of who I was and just became a baby feeding machine. I just never thought of correlating depression and breastfeeding.
maria
March 19, 2014 at 9:09 am
[…] support today. The “overload of information” has brought light to the seriousness of postpartum depression […]
Ten babies, nearly two decades breastfeeding | Our Milky Way
April 13, 2014 at 10:06 am
[…] who has done her own studies on depression and breastfeeding, says the important thing is to strengthen the mother-baby bond. If breastfeeding is important to a […]
Should Breastfeeding Moms Stay On Antidepressants? Why These Researchers Say Yes | Times of News | Online breaking and Latest News From USA
April 15, 2014 at 9:41 pm
[…] sobre depressão e amamentação pregam que o importante é fortalecer o vínculo mãe-bebê. Se a amamentação é importante para […]
Mães que usam antidepressivos devem continuar amamentando? | Ponto Vida - O seu portal de Saúde
July 1, 2014 at 6:06 am
[…] of depression or other mood disorders, and that, for some women, weaning may be the answer. As this post on the Academy of Breastfeeding Medicine blog states: If breastfeeding is the lifeline that is holding her and her baby together, then […]
Breast is not always to blame | The Boob Geek
September 10, 2014 at 9:02 pm
[…] sobre depressão e amamentação pregam que o importante é fortalecer o vínculo mãe-bebê. Se a amamentação é importante para […]
Mães que usam antidepressivos devem continuar amamentando? | Movimento Mama que te Faz Bem
February 24, 2015 at 2:38 pm
I am still breastfeeding at 19 months. I stay at home with my daughter and I love being able to still breastfeed her. However since I have been breastfeeding I have horrible mood swings. I find myself angry with my husband and other people. Having a baby is stressful but I have been wondering for awhile if breastfeeding is somehow contributing. It feels like I am having one long PMS episode-like a over a year long. Looking back almost a decade I realize it was similar when i breastfed my now teenage son. I love breastfeeding but have started cutting back since baby is getting older. Hopefully more research is done in this area so that mothers wont have to suffer so much in silence over this.
Mimi Mandrake
December 5, 2015 at 1:09 pm
I also think you can not look at this with-out consideration of how physiological or not the woman’s labour and birth were> As induction is no natural oxytocin as it does not cross the blood-brain barrier to effect maternal bonding but locks up oxytocin receptors on the uterus………………
Denise Hynd
January 10, 2016 at 6:08 pm
I had to wean my son abruptly at 17 months because of being prescribed a medicine which could come through in breast milk. Neither of us wanted this and I was very depressed for several months.
B
January 11, 2016 at 3:18 am
[…] baby. Breastfeeding releases prolactin and oxytocin, two major contributors to milk production. Depression during breastfeeding can occur, but it is most often reported when moms wean their baby too […]
Postpartum Care: Loving Your Post-Childbirth Body
April 21, 2016 at 10:02 pm
[…] sobre depressão e amamentação pregam que o importante é fortalecer o vínculo mãe-bebê. Se a amamentação é importante para […]
Mães que usam antidepressivos devem continuar amamentando? – Temos que falar sobre isso – TQFSI
June 4, 2016 at 2:32 pm
[…] turns out some women have much lower levels of oxytocin than others, which can be measured in pregnancy and could even predict post natal depression […]
The New Blue | Dev
August 3, 2017 at 8:53 am
[…] I had a bucket list I was not able to check off. When I was seven months pregnant, I wanted to do a photo shoot wearing nothing but a bandeau bra on top to show my beautiful belly. I was waiting ‘til my 9th month as supposedly it was that time when my belly was at its biggest. That moment never came as I gave birth prematurely. My baby at that time, wasn’t doing well. She cannot thermo-regulate so she needed to stay at the incubator for three weeks. I had to give her my energy so we did kangaroo mother care for 6 to 8 hours every day. She didn’t know how to properly breastfeed so we had to teach her for a very grueling three weeks. Plus, I had to think of the bills and loans and debts that went with hospitalization. But, I’d like to think that breastfeeding, in a way, played a large part in keeping me sane. Of course it was taxing and tiring and I had a really big responsibility to play. If I don’t make enough milk, my baby won’t eat. But this big responsibility, together with God, always on my side, helped me get my act together and make it ‘til everything went fine. Related: Breastfeeding and depression: It’s complicated | Breastfeeding Medicine […]
Top 5 Myths on Breastfeeding – The Quirky Freelancer
February 27, 2018 at 10:47 pm
[…] Related: Breastfeeding and depression: It’s complicated | Breastfeeding Medicine […]
Top 5 Myths on Breastfeeding – The Quirky Freelancer
February 27, 2018 at 11:15 pm
My daughter suffered from chronic depression after her fathers death. Suffered PTS. Only used natural and diet for few yrs. Was intoduced to Gaba which really helped her. After 4 months frw pregnant and stopped using anything. Baby now 10 weeks and breastfeeding. Is a very relaxed mom but she can feel bouts of depression coming on. Can she use Gaba for anxiety again if breastfeeding. Concerned over growth hormone. Or what other alternative. Doesnt want to stop breastfeeding. Very healthy happy baby.
Jenny Sprackett
March 7, 2018 at 1:57 am
[…] sobre depressão e amamentação pregam que o importante é fortalecer o vínculo mãe-bebê. Se a amamentação é importante para […]
Mães que usam antidepressivos devem continuar amamentando? – Eu Apoio Leite Materno
June 20, 2018 at 4:31 pm